If you’re holding a hot water pad around your stomach or taking constant painkillers during your periods because of bad period cramps, then this blog can be helpful for you. Period pain is a common problem that women are going through which should not be normalised where you are suffering from pain without telling anyone (each and every month).
Sometimes it can be normal period cramps which cause mild discomfort, but some may feel discomfort at such a level that their routine life is badly affected (you can’t continue with your daily work, exercise, travel, etc.) because of this. If you are also facing this kind of issue then don’t worry, here is some advice and info given which can help you with your problem.
What this blog contains:
As mentioned earlier, if you are having painful periods, which is scientifically called dysmenorrhoea, then you are in the right place. After reading this blog, you can easily understand about dysmenorrhoea, why it happens, the main cause, a few advice on how to resolve it, and further info about its complications, which may help you understand your body.
What Is Dysmenorrhea?
Primary Dysmenorrhea (Common Menstrual Cramps)
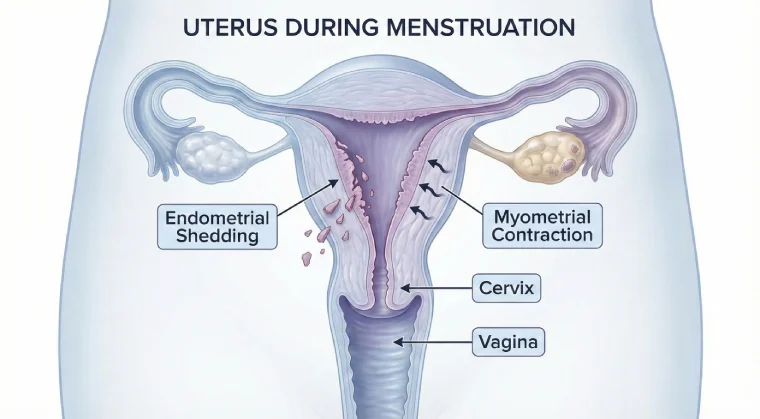
Dysmenorrhoea, in which cramps are due to normal physiology of the cycle, has no other pathological cause. As the uterus contracts during the cycle to shed its lining because of high levels of prostaglandin (it’s a local hormone which helps in the contraction of the uterus). In primary dysmenorrhea, spasmodic and centralised pain will occur, which starts the day before menses or on the same day of menses. Primary dysmenorrhea usually occurs in young girls. Up to 50–90% of menstruating women experience dysmenorrhea.
Secondary Dysmenorrhea (Pain Due to Medical Conditions)
Dysmenorrhoea, which occurs due to further pathology of the reproductive system, like endometriosis, adenomyosis, fibroids, pelvic inflammatory disease, cervical stenosis, etc.
In secondary dysmenorrhoea, pain is a localised type that starts to occur many days before the day of menses and lasts for many days. Secondary dysmenorrhoea usually occurs in women who are above 30 years of age.
What Causes Severe Period Pain?
During menstruation, blood and tissue (which also contain unfertilised egg) is shed off from the vagina of a lady. This shedding of the uterus lining and blood occurs because of the contraction of the uterus. Prostaglandin is a local hormone that is released few times before menses, and this high level of prostaglandin leads to contraction of the uterus, which leads to tightening of the lower abdomen and feels like discomfort.
Few women feel more pain while other feels less pain which may be due to various levels of prostaglandin person to person (it depends on body physiology).
Medical Conditions That Cause Secondary Dysmenorrhea
Secondary dysmenorrhoea occurs due to any pathological conditions of your reproductive organs. A few conditions are mentioned below:-
1. Endometriosis:
It is the most common condition that can lead to secondary dysmenorrhoea in females. In endometriosis, endometrial tissue grows outside the uterus, i.e. the fallopian tube, ovaries, etc. Shedding of this endometrial tissue causes severe pain and scarring.
2. Adenomyosis:
It is another condition in which the endometrial lining of the uterus specifically grows within the muscular layer. So it can lead to profuse, painful, and prolonged bleeding during the menses.
3. Pelvic inflammatory disease:
It’s a condition in which the infection of the uterus, fallopian tube, and ovaries lead to reverse pain can occur for a prolonged period during menses and can cause pain during intercourse.
4. Intrauterine device-related pain (Copper vs Hormonal):
If any woman undergoes an intrauterine contraceptive device method for contraception, it can be the cause of severe cramps during periods (especially copper IUDs ) . On the other hand, hormonal IUDs can relieve the cramps during menses.
5. Ovarian cysts:
In this condition, the ovaries are filled with a fluid, which causes pain during ovulation. Ovulation occurs during the middle of the menstrual cycle. Ovarian cysts can be a reason for abnormal bleeding and pelvic pain during periods.
6. Cervical stenosis:
This condition can worsen the period pain as the narrowing of the cervix leads to a decrease in the outflow of blood and creates pressure, which increases pain during menses.
7. Leiomyomas (Uterine fibroids):
It’s a tumor of the muscular layer of the uterus and can be a cause of severe bleeding and dysmenorrhoea.
Symptoms of Dysmenorrhea
- Discomfort
- Pain in the lower abdomen
- Pain in the lower back
- Pain in the thighs
- Headache
- Vomiting, nausea
- Fatigue
- Bloating or abdominal fullness
The above-mentioned symptoms are commonly shared by both primary dysmenorrhea and secondary dysmenorrhoea.
Few symptoms which are seen in secondary dysmenorrhoea are:
- Pain starts much earlier and lasts longer than primary dysmenorrhea
- Heavy bleeding
- Pain during intercourse
- Irregular cycle
Who Is at Higher Risk for Painful Periods?
- Young women (adolescents)
- Women with a family history of dysmenorrhoea
- Women who smoke
- Stress and anxiety (may lead to dysmenorrhoea)
- Women who have irregular menstrual periods
- Women with other pathological conditions like endometriosis, fibroids, adenomyosis, etc.
- Early menarche ( before the age of 12 )
When Should You See a Doctor?
- Severe discomfort because of pain, so that you can’t unable to do your normal work
- Pain that is progressive (increases with time )
- Pain starts to occur earlier than menses and stays longer.
- If you have conditions like pelvic inflammatory disease, PCOS, uterine fibroids, etc.
- pain during sexual intercourse
- progressive worsening pain over several cycles
How Is Secondary Dysmenorrhea Diagnosed?
As primary dysmenorrhea does not have any pathology therefore no diagnostic method is required. As in secondary, there is pathology of female reproductive organs; therefore, diagnostic methods are needed to perform.
First, you have to tell your doctor about your symptoms, then an examination is performed by the doctor, which involves the inspection of the female genitalia. During examination, your vagina, cervix is inspected as if any infection is there or not and a speculum is placed so that view get more clearer. If the doctor suspects any pathology, they can take a sample of vaginal fluid for further testing to get a better diagnosis.
Medical history:
- Duration and nature of pain
- History of menstral cycle
- Symptoms
- Family history
- Previous surgeries or infection
Systemic examination:
- Inpection of female genetilia like vagina, cervix, uterus to look any infection or pathology.
Imaging and other methods are also used to better understand the pathology of the uterus and ovaries, as these organs are not inspected during examination.
Ultrasound: High-frequency sound waves are emitted through the body, and in return, echoes are produced, which are analysed. These echoes are used to create an image of the internal organs of the body. This helps in the better examination of the uterus and ovaries.
Hysteroscopy: Through this procedure, a hysteroscope (a thin lighted telescope-like instrument )is inserted into the body via the cervix to look for any abnormalities in the uterus.
Laparoscopy: An incision is made in the abdominal region through which a laparoscopy is inserted into the body. This laparoscopy has a light and a camera which helps in better vision of the uterus to diagnose any pathology.
Best Treatment Options for Period Pain
1. NSAIDs (Ibuprofen, Naproxen)
As we understand, the production of prostaglandin causes period cramps. These drugs help in reducing the level of prostaglandin by inhibiting the COX enzyme, which is responsible for the production of prostaglandin. By this mechanism, these drugs help in reducing pain during periods.
These are over-the-counter drugs that can be available at a normal pharmacy. E.g., Ibuprofen, naproxen
2. Hormonal Birth Control Pills
It includes birth control pills, which can be given to relieve period pain as these pills also help in reducing the level of prostaglandin, and it may also cause thinning of the uterus lining, which causes less bleeding and less pain.
3. Antispasmodic Medicines
These groups of drugs help in relaxing the uterine muscles, which helps in reducing period pain. E.g., Hyoscine, drotaverine
Natural Remedies for Period Pain Relief
1. Herbals teas:
Chamomile tea: Add 3 to 4 chamomile flowers to a cup of hot water and boil it for 5 to 7 minutes. You may add lemon or honey for flavour accordingly. It contains anti-inflammatory and anti-spasmodic properties, which help in reducing the level of prostaglandin and relieve pain.Ginger tea: Add a few ginger to a cup of hot water and boil it for 4 to 5 minutes. It helps in pain relief during the period as it reduces levels of prostaglandin.
Peppermint tea: Add a few leaves of peppermint to a cup of boiling water and keep it for 4 to 5 minutes. You may add honey or jaggery to your taste.
2. Heat therapy:
You can use a heating pad or hot water bottle for pain relief. Putting a heating pad on your lower abdomen for 20 minutes helps in increasing circulation in the lower abdomen, relaxing uterine muscles, and improving the condition.
3. Proper hydration:
Drink warm water, which helps in reducing bloating, which usually occurs during menses.
Other ways to get relief from dysmenorrhoea:
- Meditation: Deep breathing practice helps in reducing stress, which ultimately helps in improving period cramps.
- Moderate exercise or yoga: Moderate or gentle exercise helps in increasing blood circulation and improves period cramps.
- Get vitamin D from sunlight. As it’s a low level can contribute to period cramps.
- Eat anti-inflammatory food, i.e., omega-3 fatty acid-rich food, magnesium-rich food, and vitamin B1-rich food.
- Avoid caffeine.
- Avoid smoking and alcohol.
- Avoid junk food.
- Sleep optimization
Real Case Example: Primary Dysmenorrhea in a 19-Year-Old
Ms X , a 19 year of female come to OPD with complaint of pain in lower abdomen, cramping sensation in thigh and legs, vomiting, diarrhoea during 1st of menstrual cycle . there is family history of dysmenorrhea and these painful periods effect her daily life activities as well . she complaint of heavy blood flow during 1st and 2nd day of menstrual cycle.
According to the given history case of primary dysmenorrhea most probably.
Treatment plan:
- NSAIDS ai onset of pain ; to suppress ovulation combined oral contraceptive pills are given
- Heat therapy , dietary modification, stress management techniques, structured exercise.
- Follow up after 6 month
Frequently Asked Questions
Q1 Is severe period pain normal?
Ans if this pain during menses is interferes with normal daily lifestyle activities then its not normal. Mild discomfort in lower abdomen is common.
Q2 When should I see a doctor about period pain?
Ans also explained above as well in the blog. You need to seek doctor’s help when-
1.Severe discomfort because of pain
2. Progressive pain
3. Pain starts earlier than menses and stays longer.
4. If you have conditions like pelvic inflammatory disease, PCOS, uterine fibroids, etc.
5. pain during sexual intercourse
6. progressive worsening pain over several cycles
Q3 Can diet affect my period?
Ans yes, a diet plan which is high in omega-3 fatty acids, magnesium, anti inflammatory foods etc. can reduce your pain and provide some relief. Avoid processed food.
Q4 Which painkiller work best and when should I take them?
Ans NSAIDS such ibuprofen and naproxen are consider as most effective pills. Shows their effect within 24 hours.
Q5 Does dysmenorrhea effect fertility?
Ans primary dysmenorrhea doesn’t affect your fertility. Secondary dysmenorrhea is associated with other conditions and these condition can affect fertility and requires medical attention.
Note from Femwise Health
Hope you get good info about your issue from this blog. Having dysmenorrhoea is very common, so don’t panic. Try a few natural ways to relieve pain. If you still feel discomfort, then connect with a healthcare provider who will guide you very well.
Glossary terms
- Dysmenorrhea: painful periods dur to menstral cramps in uterus.
- Prostaglandins: hormone like chemical released during menses and Cause contraction of uterus.
- Endometriosis: it’s a condition where endometrial like tissue outgrows beside uterus. E.g. most common site id fallonpian tube and ovary
- Laproscopy: it is a minimal invasive surgery used to diagnose pelvic condition and help in making better treatment.




